The blood–brain barrier: the final frontier?
Technology enabling the penetration of substances through the blood–brain barrier is a breakthrough development since it allows for a targeted drug delivery to the brain.

![]()
header.search.error
Technology enabling the penetration of substances through the blood–brain barrier is a breakthrough development since it allows for a targeted drug delivery to the brain.

As populations age, the prevalence of chronic diseases is rising significantly.1 Most chronic conditions are age-related and are therefore a major consideration under any healthcare system. However, as many of the chronic degenerative diseases are located in the brain, they are difficult to target even by modern medicine. Progress in treating diseases such as Parkinson’s, Alzheimer’s, and multiple sclerosis has been slow.
Why is it so difficult to produce medication that would directly target the brain? One of the reasons seems to be the existence of the so-called blood–brain barrier, also referred to as the BBB, which prevents many substances circulating in the bloodstream from entering the brain. While such a protection is vital to the brain, the flipside is that it is extremely difficult for medications targeting the brain to reach their destination in therapeutically active concentration.
Alzheimer's, Parkinson's, and other degenerative brain diseases are becoming a major factor lowering the quality of life for many elderly people. Finding a way to deliver medication directly to the brain could significantly accelerate progress toward solutions to fight those diseases.
Why do we need the blood–brain barrier?
The blood–brain barrier acts as an additional boundary between the circulating blood and the extracellular space of the brain. The barrier is highly selective, which means that it only allows certain substances to get from the bloodstream into the brain, which helps protect the brain from toxins, pathogens, and even circulating neurotransmitters (e.g. glutamate) that can be potentially damaging to neurons if their levels get too high. Only water, certain gases (e.g. oxygen), and lipid-soluble substances can easily diffuse across the barrier (other necessary substances like glucose can be actively transported across the blood–brain barrier with some effort).2
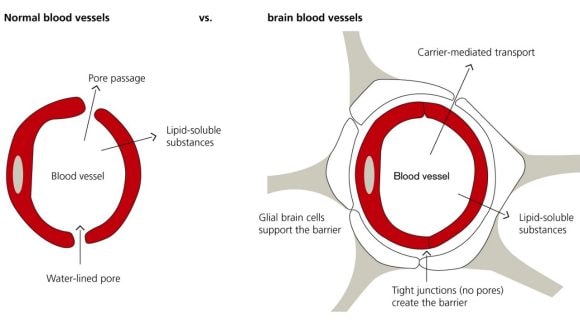
As mentioned, the purpose of the blood–brain barrier is to protect the brain against circulating toxins or pathogens that could cause brain infections, while at the same time allowing vital nutrients to reach the brain.
Its other function is to help maintain relatively constant levels of hormones, nutrients, and water in the brain – fluctuations in which could disrupt the finely tuned environment.
So what happens when the blood–brain barrier is damaged or somehow compromised?
One common way this occurs is through bacterial infection, as in meningococcal disease. Meningococcal bacteria can bind to the endothelial wall, causing tight junctions to open slightly. As a result, the blood–brain barrier becomes more porous, allowing bacteria and other toxins to infect the brain tissue, which can lead to inflammation and sometimes death.
It is also thought that the blood–brain barrier’s function can decrease in other conditions. In multiple sclerosis, for example, a defective blood–brain barrier allows white blood cells to infiltrate the brain and attack the functions that send messages from one brain cell (neuron) to another. This causes problems with how neurons signal to each other.3
How can we get through the blood–brain barrier?
The blood–brain barrier is generally very effective at preventing unwanted substances from accessing the brain. As a result, the vast majority of potential drug treatments are not able to cross the barrier, which poses a huge impediment to treating mental and neurological disorders.
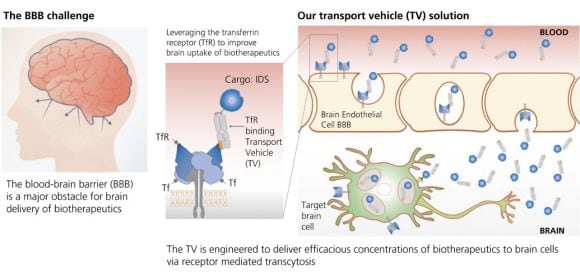
One possible way around the problem is to “trick” the blood–brain barrier into allowing the passage of the drug. This is the so-called Trojan horse approach, in which the drug is fused to a molecule that can pass the blood–brain barrier via a transporter protein.
A different approach is to temporarily open the blood–brain barrier using ultrasound.4
To reach a more uniform distribution of medication in the brain, as well as for safety reasons, primarily non-invasive techniques are currently targeted for development.

Denali Therapeutics – a platform built around crossing the blood–brain barrier
As a company working on a broad platform for brain delivery, Denali Therapeutics has entered into collaborations with Biogen, Takeda, and Sanofi.5 This should not come as a surprise, as a transport mechanism combined with an already established pathway of a drug can offer mutual benefit to all partners.
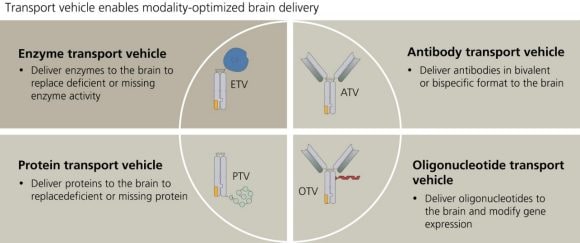
As amazing as it may sound, Denali Therapeutics works on brain delivery in four different classes of medications. Each of these transportation modalities is a platform in itself since it can potentially be applied to many different individual medications.
Crossing the blood–brain barrier may accelerate treatment of neurogenerative diseases
When we invest in the digital health theme, we are looking for platform solutions that can potentially offer a much better outcome for patients. Compared to other illnesses, degenerative brain diseases are an area of very high unmet need. A healthy brain is considered a major factor in judging quality of life.
Progress in the development of new pharmaceuticals for the treatment of the brain in aging, including Alzheimer’s disease, has been extremely slow because the products of biotechnology, recombinant proteins or gene therapies, are all large molecule pharmaceuticals that do not cross the blood–brain barrier. Back in 2019, there was not a single recombinant protein approved by the FDA for the treatment of Alzheimer's disease, or any other brain disease, wherein the drug has to enter the brain via the blood–brain barrier.6
The blood-brain barrier is a wonderful evolutionary development aimed at protecting our precious brain from damage; however, it also keeps out medication from reaching the brain. A technology that can make the blood–brain barrier permeable with as much precision as possible could rightfully be considered a key platform enabling us to cross this final frontier, for the good of society.

CFA, Senior portfolio manager, Thematic Equities
Thomas Amrein (MSc, CFA), Director, is a Senior Portfolio Manager and Lead Manager of the Digital Health Equity strategy. Before that, he focused on the US healthcare sector, managing the USA Growth Opportunities Equity strategy. He became Lead Portfolio Manager of the Credit Suisse Global Biotech Innovators Equity strategy in 2016. Thomas joined Credit Suisse Asset Management, now part of UBS Group, in 1996. He has covered the healthcare and other sectors for over 20 years. Thomas holds a master’s degree in Business Administration from the University of St. Gallen and is a CFA charterholder. He also attended postgraduate courses in biotechnology at the University of Basel and ETH Zurich.